I have the extremely good fortune of being one of the first people in the world to receive the Dexcom G6, the latest in continuous glucose monitoring (CGM) technology. After spending almost two years eagerly anticipating its FDA approval, I could scarcely believe that I finally had it in my hands when it first arrived a few weeks ago.
I am partway through my second-ever G6 sensor, so I’ve had enough time to come up with some initial opinions on the system as a whole compared to the G5.
Let’s start with what I knew going into the first insertion of the G6. I knew that the transmitter would have a sleeker profile than the G5. I also was aware that the insertion process would be much more streamlined – all I would need to do is push a button and it would be on my body. Plus, the G6 required 0 finger sticks or calibrations, could be worn for 10 consecutive days, and would no longer block acetaminophen (Tylenol) like its predecessors did. So far, me and the G6 were off to a solid start.
Then, it came time for me to actually put it on. Rather then end my current session with my G5, I decided to leave it on so I could see how accurate it was compared to the G6.

I was amazed by how easy it was to insert the G6. All I had to do was input a 4-digit code located on the sensor into my receiver. Once the code was accepted, I peeled the adhesive off the sensor, placed the system on my abdomen, folded the orange safety clip until it snapped off, and pushed the big orange button. I cringed when I did it for the first time; truthfully, I was prepared for it to hurt. It made a ka-shunk sound as the sensor inserted itself into my skin, and I…didn’t feel a thing. I marveled at how ridiculously comfortable it felt as I snapped the sleeker transmitter into place. I pressed one more button on my receiver to get the sensor warmed up, and that was it. Once two hours elapsed, my G6 system would be fully operational and could determine my blood sugar without requiring manual calibrations.

While it felt great to know that I didn’t need to worry about calibrating my new device, I was more interested in seeing how well it matched up with my G5.
And I was a little let down…at least, I was in the beginning.
Initially, I was not impressed at all by the G6’s reports. They matched pretty damn closely with my G5. I was beginning to wonder whether the technology really was that excellent, and then my G6 proved to me that it was, indeed, kind of a big deal.
That moment came when it caught a low blood sugar sooner than my G5. I was feeling the early signs of a low, so it wasn’t much of a surprise when it alarmed. But what was particularly neat to me was that it was able to tell me that a serious low blood sugar (below 55 mg/dL) was oncoming in the next 20 minuets or less. In other words, it knew that I needed to treat my blood sugar right away to prevent a more urgent hypoglycemic event. That predictive feature was definitely a pleasant surprise.
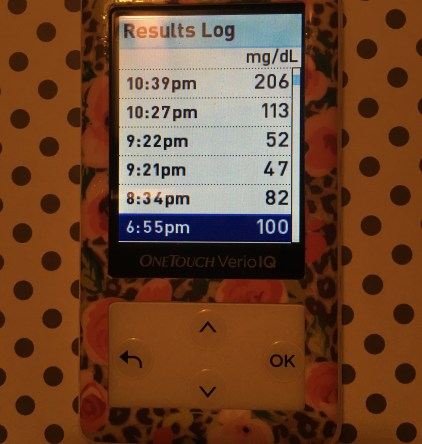
As I wore my first G6 sensor for a few more days, it seemed to adjust better and better to my body. As evidenced in the above picture, it proved to be spot on when I compared it to the blood sugar readings I got from my meter. There’s absolutely still a bit of the classic CGM lag, as it takes about 15 minutes or so to catch up to what’s actually going on in the body, but that was to be expected.
I’m already on second sensor and I think it’s safe to say that I’m sold on the G6. But I don’t think that any product comparison/review is complete without a list of pros and cons, so here’s what I’ve come up with:
Pros of the G6 (compared to the G5)
- Slimmer transmitter profile
- 0 fingerstick calibrations (which I really loved when I didn’t have to wake up in the middle of the night to calibrate a sensor I inserted before bed)
- Predictive low feature
- Modern touchscreen receiver
- Absolutely painless and foolproof application – honestly, it was THAT good that it might win me over from the G5 if that was the sole difference between the two
Cons of the G6 (compared to the G5)
- Clunky applicator – as many other members of the DOC have noted, the system is comprised of a lot of plastic. Probably not very environmentally friendly. I wish it was possible to recycle it somehow
- Automatic expiration after 10 days – with the G5, you could restart a sensor after a week had elapsed, and in theory, you could use the same single sensor more than once for a few weeks in a row. The G6 automatically shuts down after 10 days, so you’re forced to put on a new sensor. This medical device is already pretty expensive, and you could at least get your money’s worth with the G5
- No super noticeable improvement in blood sugar reporting capabilities
The bottom line is that the G6 is unquestionably an upgrade in diabetes technology. It requires fewer blood sugar checks and allows for greater discretion with its smaller size. The G6 is far from perfect, but it’s still a valued component of my diabetes toolkit. I’m excited to continue on this journey with it and discover just how much it helps me take the best possible care of myself.