Say hello to my new little friend…Baqsimi!
For anyone who may be unfamiliar with Baqsimi, it’s a relatively new form of glucagon that comes as a nasal spray. I haven’t had to use it yet (and I hope that I don’t ever have to, really), but there’s a lot of pros to Baqsimi when comparing it to a traditional glucagon kit:
- It’s shelf-stable – it doesn’t have to be refrigerated.
- It doesn’t expire until 2.5 years from now.
- It’s completely ready to go as-is, no mixing or measuring needed.
- It’s compact and totally portable.
- It’s easy to use (and understand how to use!).
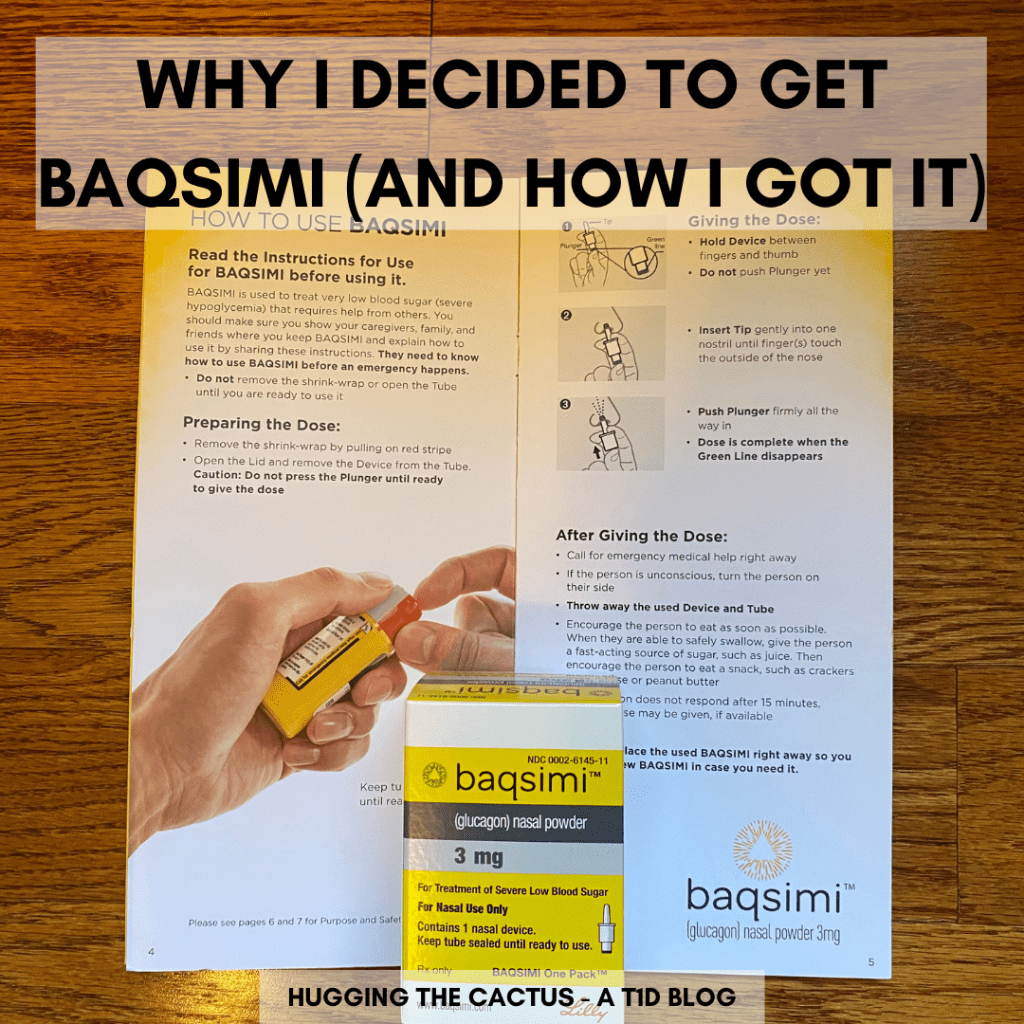
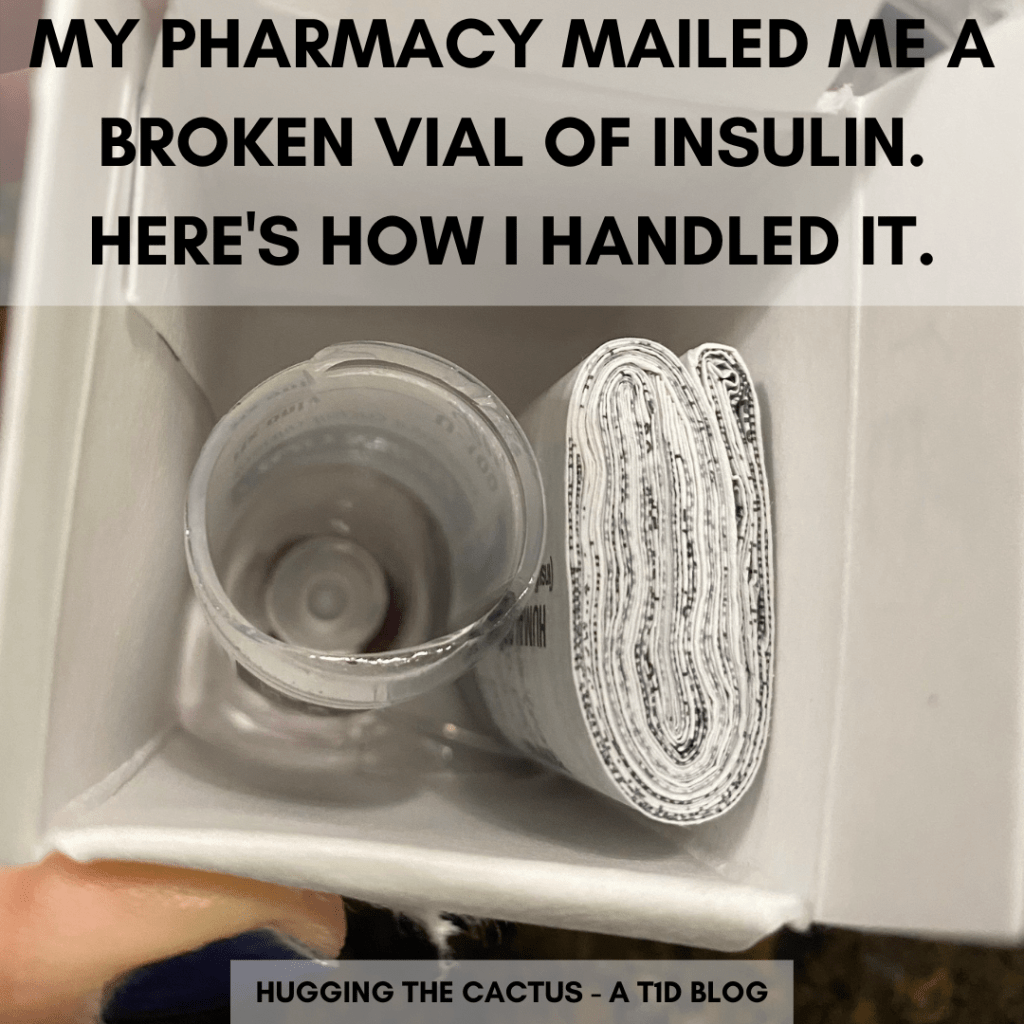
All of those factors contributed to my decision to finally pull the trigger and ask my endocrinologist about writing a prescription for me. It’s not that I’m suddenly worried that I’ll need Baqsimi; for me, it’s more of a peace-of-mind situation. I always thought that my glucagon kit was next to impossible. Sure, I know how to use it, but I have to refresh my memory every so often because there are so many steps involved in the process: inject the syringe into the vial, mix the contents, wait for the glucagon to turn clear, stick the syringe back into the vial, withdraw the liquid, and then finally do the injection…there’s a lot going on there. And if I actually did need glucagon one day due to a severe hypo, I wouldn’t exactly be able to easily walk whoever I was with through the process because I’m sure I’d be totally incapable of doing so (depending on how bad my symptoms were).
It’s just a lot to ask of every single one of my family members and friends to know exactly how to inject glucagon into me in the event I ever needed one of them to do that, so having Baqsimi on hand takes so much of that fear and anxiety away.
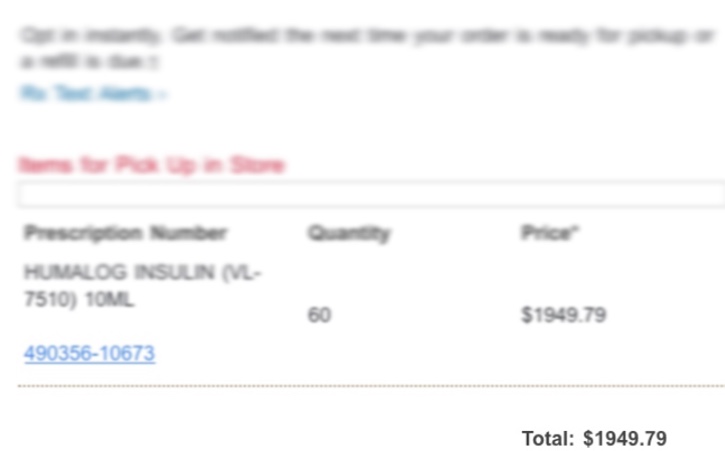
And the icing on top of the cake is that it was super easy for me to get Baqsimi…like, it only took a few hours, which is amazing. All I did was reach out to my endocrinologist’s office using their online messaging system, ask my doctor for a script, and…bam. It was sent into my local pharmacy, and before long, I was cruising through the drive-thru with my dog to pick it up. I’m lucky, too, because all I had to pay was $25, thanks to my insurance (sometimes, it’s not as bad as I think it is).
Twenty-five bucks for peace of mind and a life-saving medication…that’s something I can get behind. I’m glad Baqsimi has finally joined my diabetes toolkit.