It was the perfect storm.
My Omnipod’s adhesive was damp from the shower. I was putting a pair of pants and not paying any mind to the pod I’d only been wearing for about 12 hours.
It’s no wonder that I brushed the fabric of my pants up against my pod in precisely the wrong way.
I heard the telltale sound of adhesive tearing off my skin and cursed before looking down to inspect the damage.
I expected to see a pod dangling on my leg by a thread, but instead I noticed that the adhesive around the cannula-end of the pod (the important end) still seemed totally stuck to my skin. It was the opposite end that was in trouble and definitely needed taping up if I hoped to save the pod.
So while I waited for my pod’s adhesive to completely dry from the shower so I could check it out further, I pondered: Do I run the risk of keeping this pod on, even though its security was significantly decreased? Or do I err on the side of caution and replace it, and enjoy the peace of mind that comes with a freshly applied pod?
Both options had pros and cons.
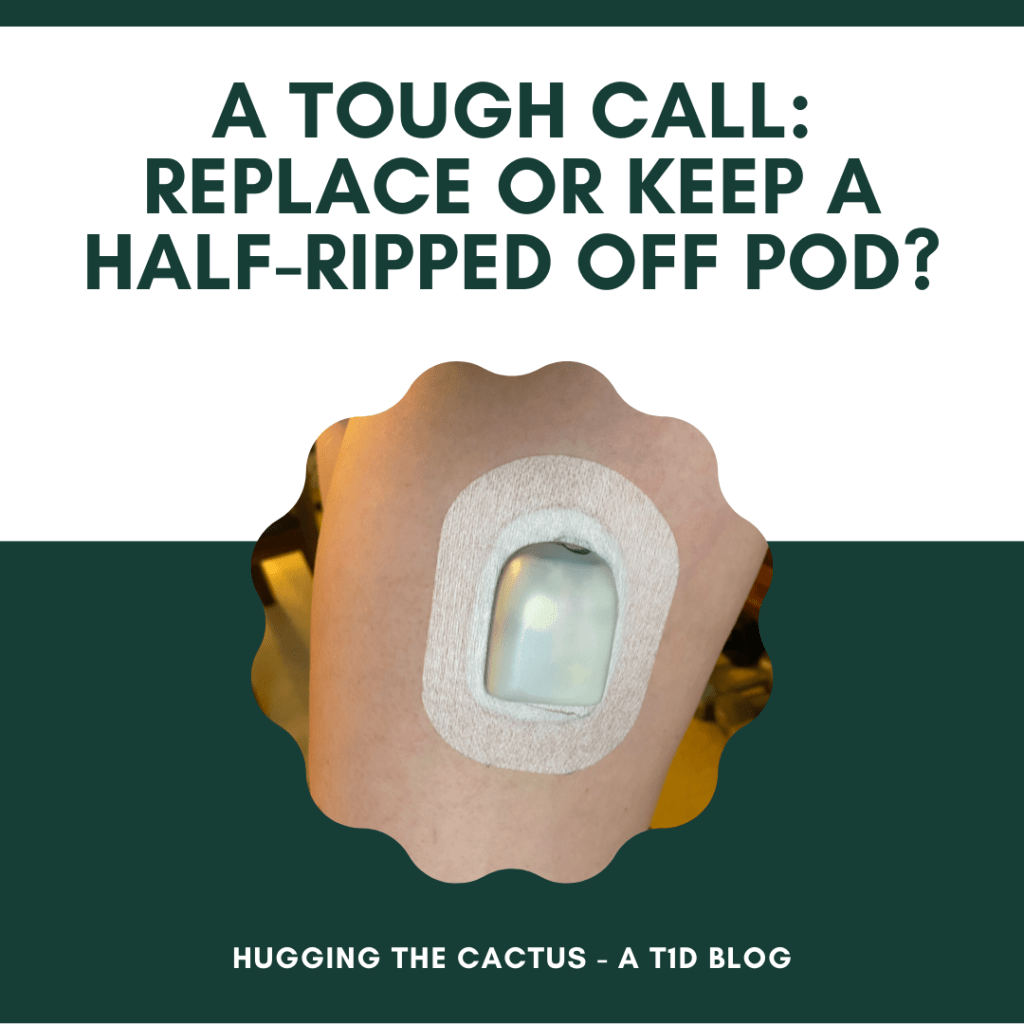
If I kept the pod on, my blood sugars might start to run high because I couldn’t say with 100% certainty that the cannula was still inserted in my skin. It looked like it could be, but the sound of half the adhesive ripping off made me suspicious. But if I replaced the pod, I would be wasting all the insulin I had just put into it the night before, which was a thought that was difficult for me to stomach.
I decided that the more favorable option to me was keeping the pod on, so once I knew it was dry, I added a little extra security by applying a PodPal (an Omnipod-shaped adhesive overlay meant to reinforce a pod’s stickiness) around it. As of this writing, only time will tell whether this was the right call to make, but my point in sharing this story is that this is an example of just one of the many judgment calls that people with diabetes have to make on pretty much a daily basis. This single decision took up mental energy and time that I would’ve rather used at work, or for chores around my house, or for just about anything else – but instead, diabetes had to be at the forefront of my thoughts and actions because it often demands just that much attention.
That’s why it’s kind of staggering to know that people with diabetes make around 180 decisions per day...with that in mind, there’s no doubting that diabetes is a condition defined by choices made. No matter how big or small – even as tiny as choosing whether or not to replace a pod – they all add up together to determine long-term health outcomes, and that in itself is a very big deal.