(Gotta give credit where credit is due on inspo for this blog post’s title – Judith Viorst authored the children’s book Alexander and the Terrible, Horrible, No Good, Very Bad Day in 1972 and a movie that was loosely based on it came out in 2014. I admit that I’ve seen neither but as someone who has appreciation for books and movies, I can at least claim an awareness of both and a deep appreciation for such a memorable title.)
At the end of July, I had my worst 24 hours of diabetes in literal years.
I’m being a little dramatic, but really, everything that could go wrong pretty much did. And what made it that much worse is that it just happened to coincide with my girls’ weekend with my college friends.
It all started after dinnertime. I had flatbread from a local restaurant that I frequent, and I substituted traditional crust in favor of cauliflower crust – my hope being that this would have less of an impact on my blood sugar levels.
No such luck. In the 3-4 hours post-dinner, my blood sugar steadily climbed, reaching a peak of the low 300s at its highest. It just didn’t make sense! I had 4 pieces of flatbread. They weren’t massive. Veggies were the only topping. Maybe it was my pod? When I went to check my PDM to see how much insulin I had on board for what felt like the fiftieth time that evening, I discovered that I’d been burning through so much insulin that I only had a few units left in the pod, meaning that I’d definitely have to change it before I went to bed to ensure I didn’t run out of insulin overnight.
I was super annoyed as a result of my hyperglycemic state and the need to do a premature pod change, but apparently also exhausted by the ordeal as I lapsed into an early sleep in my armchair while my friends stayed up. By the time I snapped out of my slumber, I was groggy, thirsty, and upset that my diabetes was affecting my ability to hang out. When we all turned in for the evening around midnight, I went to bed hoping that my mood and blood sugars would be turned around by the time I woke up in the morning.

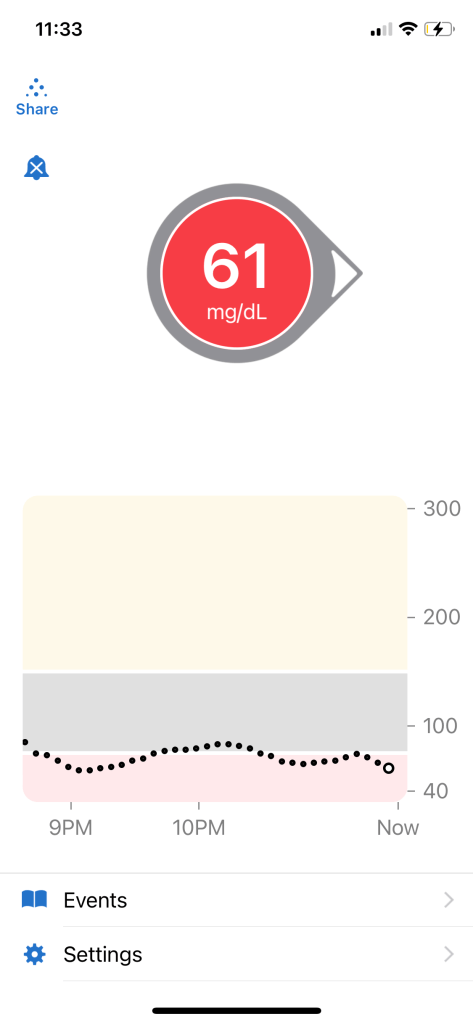
Except they didn’t. I woke up in the middle of the night with not one, but two separate low blood sugars. My broken sleep combined with the wild oscillations of my blood sugar caused me to roll out of bed with a stinging pain in my eyes and a defeated spirit that I tried my best to hide from my friends, but to no avail. In fact, I ended up in a heap on the floor, crying to them as I apologized for my grumpy mood and attempted to explain to them what had gone wrong in the last 12 hours. They were all very understanding and supportive, but I felt horrible for being so temperamental and curt with them; after all, none of this was their fault. I promised them that I’d cry it out, wash my face, get dressed, and spend the rest of my time with them with an adjusted attitude.
This mostly worked – we were able to enjoy bagels and lattes for breakfast, as well as a long walk in the first truly gorgeous morning of weather we’ve had since May. My attention was absolutely still partially focused on my diabetes, especially since bagels are notoriously tricky to bolus for, but my resulting spike from indulging in one wasn’t too bad since it was offset by the walk.
By the time my friends departed, my blood sugar was mostly back under control. This must be when things started turning around for me, right? Wrong! As I cleaned up my condo, I ripped my pod – the one that I had just applied the previous evening – clean off my leg. Cursing, I tried to calm myself down because this was something I could easily fix. I decided to call my boyfriend while I did the pod change routine, which was yet another mistake on my part as I accidentally deployed the cannula before the pod was even on my body.
It was like a comedy of errors. I shouted – yes, legitimately yelled – to my bemused boyfriend that I had to go. I needed to get this pod change done and over with, distraction-free. So I repeated the process, only to find that pod #2 was unusable because the cannula was poking out.
Was the universe laughing at me at this point? It sure felt like it.
Third time’s the charm, I told myself as I audibly sighed out of frustration. And thank goodness that it really, truly was – the third attempt at putting a new pod on was the one that did the trick. I remember falling back in my chair after the pod was securely attached on my body. The rollercoaster blood sugars and the unpredictable technology demands truly drained me, and this was just one 24-hour window of dealing with diabetes.
Thank goodness most days aren’t like this terrible, horrible, no good, very bad diabetes day!